IT Solutions for Healthcare and Medical Clinics in Saudi Arabia
Introduction
Saudi Arabia's healthcare sector is growing at a pace that most clinic management systems were not built to handle.
Vision 2030's health sector targets include significant expansion of private healthcare capacity, mandatory health insurance coverage for Saudi nationals, and the digitisation of health records across the Kingdom. The Ministry of Health (MOH) and the Central Board for Accreditation of Healthcare Institutions (CBAHI) have both incorporated IT standards into their accreditation and inspection frameworks.
For private clinics, polyclinics, specialist centres, and medical groups, the operational and regulatory IT requirements are more demanding than they were five years ago and will be more demanding still in five years.
Many healthcare providers in Jeddah, Riyadh, and across Saudi Arabia are still running on paper appointment books, manual patient record files, and WhatsApp-based patient communication. Some have adopted basic practice management software but have not integrated it with their billing, their clinical records, or their insurance processing workflows.
This guide covers the specific IT systems that address the most important operational and compliance challenges for Saudi healthcare providers, what each system does, what the Saudi-specific requirements are, and how to prioritise investment.
The Operational IT Problems Saudi Healthcare Providers Face
Appointment Scheduling That Does Not Scale
A clinic that books appointments by phone, or through a WhatsApp chat managed by a receptionist, works adequately at low volume. As the clinic grows, the same system creates bottlenecks: phone lines are busy, patients wait too long for confirmation, double bookings occur, and the receptionist is handling 50 messages a day rather than supporting patients in the clinic.
Saudi patients increasingly expect online booking. The ability to book an appointment at 11pm on a Thursday without calling anyone is now an expectation across most healthcare segments, particularly among younger patients and those with demanding schedules.
Paper Patient Records That Create Risk
Paper-based patient records create four specific problems. They are physically insecure: anyone with access to the filing area can read any patient's records. They are operationally slow: pulling and refiling a patient chart before every consultation adds time to every clinical encounter. They are incomplete: notes made in different encounters by different clinicians are not always filed together, and critical clinical information may be missed. And they create regulatory risk: CBAHI accreditation standards require that patient records are complete, accessible, and securely maintained.
Electronic Medical Records (EMR) solve all four problems simultaneously.
Insurance and Billing Workflows That Are Manual and Error-Prone
Insurance claim processing is one of the most time-consuming and error-prone administrative tasks in Saudi healthcare. Manual claim preparation, submission, rejection management, and follow-up consumes significant administrative capacity and produces delayed revenue.
Rejection rates for manually prepared claims are typically 15 to 25 percent in Saudi healthcare. Each rejection requires someone to identify the error, correct it, and resubmit. For a mid-sized clinic processing hundreds of claims per month, this is a significant ongoing cost.
No Visibility Into Clinic Performance
Most clinic managers can tell you how many patients they saw this week. Very few can quickly tell you which appointment types generate the highest revenue per hour, which clinicians have the longest patient wait times, which insurance payers have the lowest claim acceptance rates, or what the average patient-to-second-visit conversion rate is.
Without this data, operational decisions are made by intuition. The clinicians who seem busiest get more resources, whether or not their contribution to the clinic's financial health justifies it.
The IT Systems Saudi Healthcare Providers Need
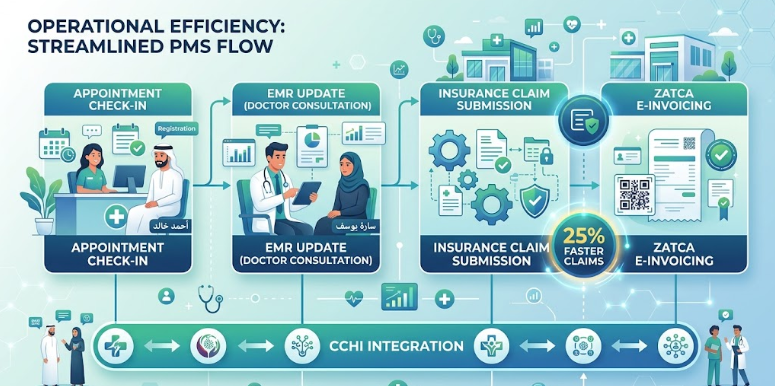
1. Practice Management System (PMS)
A Practice Management System is the operational core of a clinic. It handles appointment scheduling, patient registration, billing, insurance claim management, and basic reporting.
For a Saudi clinic, the PMS needs to include several specific capabilities. It must integrate with the Saudi insurance ecosystem, including the ability to submit claims to the major Saudi insurance companies in the required electronic format and manage the rejection and resubmission workflow. It must generate ZATCA-compliant receipts for patient payments. It must support Arabic and English for both staff-facing interfaces and patient-facing documents. And it must handle the Naphcare (formerly Waseel) electronic claims submission requirements that most Saudi insurance companies now mandate.
A well-implemented PMS reduces appointment booking errors, accelerates insurance claim processing, and gives clinic management the financial data they need to run the clinic as a business rather than a clinical operation with billing as an afterthought.
2. Electronic Medical Records (EMR)
An EMR is the digital equivalent of a patient's paper chart, with significant additional capabilities. It stores the complete clinical history for each patient: diagnoses, medications, allergies, lab results, imaging reports, clinical notes, and referral history.
For a Saudi healthcare provider, the EMR needs to handle Arabic clinical notes (most Saudi clinicians document in a mix of Arabic and English), integrate with laboratory and imaging systems to receive results directly rather than requiring manual entry, produce clinical summaries in formats acceptable for insurance pre-authorisation, and maintain a complete, unalterable audit trail of every record access and modification.
The Ministry of Health's Unified Medical Record initiative and CBAHI's standards both require that patient records are complete, accurate, and securely maintained. An EMR system designed for the Saudi market meets these requirements by default. A generic system may require significant customisation.
EMR implementation requires careful change management. Clinicians who have worked with paper records for years may be resistant to the transition. The most successful implementations involve clinicians in the system selection process, provide adequate training before go-live, and allow a parallel paper/digital period during the transition.
3. Patient Engagement and Communication Platform
A patient engagement platform manages communication between the clinic and its patients across the full care journey: appointment reminders before the visit, post-visit care instructions, prescription refill reminders, annual checkup prompts, and satisfaction surveys.
For a Saudi clinic, WhatsApp integration is essential. Saudi patients communicate primarily through WhatsApp, and automated WhatsApp messages for appointment reminders and confirmations produce significantly higher response rates than SMS or email.
The platform must handle Arabic-language communications correctly. Generic patient communication tools built for Western markets often have limited Arabic support or produce poor-quality Arabic text. A tool built or configured specifically for the Saudi market addresses this.
Automated appointment reminders alone typically reduce no-show rates by 20 to 40 percent. For a clinic where an empty appointment slot represents lost revenue that cannot be recovered, this is a direct financial return.
4. Healthcare Cybersecurity
Patient health information is among the most sensitive personal data covered by the Saudi PDPL. It includes diagnoses, medications, mental health history, and reproductive health information that patients have a fundamental interest in keeping private.
Healthcare providers are a high-priority target for cybercriminals precisely because of the sensitivity of this data and the operational impact of any system outage. A ransomware attack that encrypts a clinic's EMR system does not just disrupt administration. It potentially interrupts patient care.
The specific cybersecurity requirements for Saudi healthcare providers include access controls that limit who can view which patient records (clinical staff should only access records for patients under their care), strong authentication for all clinical system access, encryption of patient data both when stored and when transmitted, regular security patching of all clinical and administrative systems, and tested backup and recovery arrangements with recovery time objectives appropriate for a clinical environment.
CBAHI accreditation standards include assessment of information security controls for patient data. Clinics that cannot demonstrate these controls risk accreditation issues.
5. Telemedicine Platform
Telemedicine has moved from an emergency measure during COVID-19 to a standard part of Saudi healthcare delivery. The Ministry of Health's telehealth regulations provide the framework within which licensed providers can offer video consultations.
For a Saudi clinic, a telemedicine platform needs to integrate with the existing PMS so that telehealth appointments appear in the same scheduling system as in-person ones, integrate with the EMR so that consultation notes are stored against the patient's record, handle payment and insurance claim processing for telehealth encounters in the same way as physical visits, and provide a reliable video connection that works on the mobile devices most Saudi patients use.
A separate, standalone telemedicine tool that does not integrate with your existing clinical systems creates more administrative work than it saves. Integration is the critical requirement.
6. Healthcare Analytics Dashboard
A healthcare analytics dashboard gives clinic management live visibility into the metrics that drive operational and financial performance:
Patient volume by clinician, by specialty, and by appointment type
Average revenue per patient encounter by payer type (insurance versus cash)
Insurance claim acceptance rate and rejection reasons by payer
Appointment utilisation rate: what percentage of available slots are filled
No-show rate by appointment type and by notification method
Average patient wait time from check-in to consultation
New versus returning patient ratio by referral source
These metrics exist in every clinic's PMS and EMR data. The problem is they require someone to extract and analyse them manually if there is no analytics layer. A connected dashboard makes them visible without any manual effort.
Saudi-Specific Healthcare IT Requirements
Several requirements are specific to healthcare IT in Saudi Arabia and must be addressed in any implementation:
CCHI compliance: The Council of Cooperative Health Insurance sets standards for insurance claim formats, pre-authorisation processes, and electronic claim submission. Your PMS must be compliant with CCHI requirements.
Naphcare/Waseel integration: Most Saudi insurance companies require claims to be submitted through electronic clearinghouses. Your billing system needs to connect to these systems.
MOH and CBAHI standards: CBAHI accreditation requires specific documentation, record-keeping, and information security controls that your IT systems must support.
Arabic clinical terminology: EMR systems used in Saudi Arabia need to support Arabic medical terminology correctly, including in structured diagnostic fields.
PDPL for health data: Health data is a specifically sensitive category under the PDPL. Consent requirements, access controls, and breach notification obligations are particularly strict for this data category.
Key Takeaways
A Practice Management System is the operational foundation for any Saudi clinic. It must include CCHI-compliant insurance claim processing and ZATCA e-invoicing from the start.
EMR systems eliminate the operational, clinical, and compliance risks of paper records. They are a requirement for CBAHI accreditation and an MOH digitisation priority.
WhatsApp-integrated appointment reminders reduce no-show rates by 20 to 40 percent. In a clinic where empty slots cannot be recovered, this is a direct financial return.
Patient health data is a specifically sensitive category under the Saudi PDPL. Access controls, audit trails, and tested backups are legal requirements, not optional security measures.
Telemedicine platforms must integrate with the existing PMS and EMR to avoid creating new administrative burden. A standalone tool that does not connect to clinical systems adds work rather than removing it.
Healthcare analytics dashboards turn the data already in your PMS and EMR into actionable operational intelligence, without requiring anyone to build a manual report.
Frequently Asked Questions
Q: Is an EMR system required for CBAHI accreditation in Saudi Arabia?
A: CBAHI accreditation standards require that patient records are complete, accessible, securely maintained, and available to authorised clinical staff when needed. Paper records can technically meet some of these requirements but make it significantly harder to demonstrate compliance, particularly around security and completeness. Most CBAHI surveyors expect to see electronic records management in place. Healthcare providers pursuing accreditation should treat EMR implementation as a practical requirement, even if it is not explicitly stated as mandatory in the current standards.
Q: How long does a clinic management system implementation take?
A: For a small to medium-sized clinic (5 to 20 clinicians), a focused PMS implementation covering scheduling, billing, and insurance integration typically takes six to ten weeks from contract to go-live. Adding an EMR module extends this to three to five months, depending on the volume of historical records to be migrated and the number of clinical integrations required. The most time-consuming element is usually insurance payer setup: configuring the specific requirements of each insurance company your clinic works with.
Q: What is the best way to migrate paper patient records to a digital system?
A: For most clinics, full retroactive digitisation of all paper records is neither practical nor necessary. The most efficient approach is forward migration: starting from the go-live date, all new patient encounters are documented digitally. For existing patients, their records are digitised when they next visit the clinic. Critical historical information (active diagnoses, current medications, allergies, relevant surgical history) is entered as a summary at the first post-migration visit. This approach spreads the digitisation work over time and ensures the most clinically important information is captured first.
Q: Can a Saudi clinic's IT system integrate with wearable health devices and remote monitoring?
A: Yes, though the complexity of integration varies significantly by device type and by the EMR platform in use. Modern EMR systems that support HL7 FHIR standards (the international health data exchange standard) can receive structured data from compatible wearable devices and remote monitoring tools. Integration with consumer devices (Apple Watch health data, continuous glucose monitors, blood pressure monitors) requires the device manufacturer to provide an API and the EMR vendor to support the data format. This is an area where the technical landscape is evolving quickly, and it is worth asking specifically about supported integrations when evaluating EMR platforms.
Q: How do we protect patient data when staff access clinical systems remotely?
A: Remote access to clinical systems requires additional security controls beyond what is needed for in-clinic access. These include multi-factor authentication for all remote access, a VPN or secure remote access solution that encrypts all data between the remote device and the clinic's systems, endpoint security on the devices used for remote access (personal devices used by clinical staff should meet defined security standards), and session recording or audit logging for remote access to sensitive patient data. Access privileges for remote sessions should be limited to the data and functions actually needed for the clinical task being performed.
Conclusion
Saudi Arabia's healthcare sector is in a period of significant change, and the IT requirements for healthcare providers are changing with it.
The combination of MOH digitisation targets, CBAHI accreditation standards, CCHI insurance processing requirements, PDPL obligations for health data, and rising patient expectations for digital services creates a complex IT requirement that is only going to become more demanding over time.
Healthcare providers that invest in the right systems now, built specifically for the Saudi market, are building the operational and compliance foundation that the next five years will require. Those that delay are accumulating regulatory risk and competitive disadvantage simultaneously.
The priorities are clear: PMS with CCHI-compliant insurance processing first, EMR implementation second, patient communication tools third, cybersecurity controls built in throughout. Each investment builds on the one before it.
Softriva provides IT solutions for healthcare providers across Saudi Arabia, including clinic management systems, web and hosting services, and the IT infrastructure that supports clinical operations. Our team is experienced with the Saudi healthcare regulatory environment and builds systems that meet MOH, CBAHI, and PDPL requirements from the design stage.
A free consultation gives you a realistic assessment of where your current IT creates clinical, operational, or compliance risk and what the most practical improvements are.

Book a Free Healthcare IT Consultation at softriva.com
